Welcome! This is a long webpage as it includes all the resources that GP practice staff may need to identify and refer eligible patients to the NHS Type 2 Diabetes Path to Remission Programme, formerly the NHS Low Calorie Diet Programme. It is designed for people who have attended or listened to one of the education sessions (includes links to videos).
You might prefer to visit the Somerset CCG TeamNet page which has these and additional resources.
We also have a range of ‘how to’ videos – accessed through a separate page.
Please email referrals to somicb.lcd@nhs.net
If you have any questions or feedback please contact Lesley Harper on lesley.harper1@nhs.net
or support@momentanewcastle.com
Note: Please DO NOT send referral or patient identifiable information to these emails
See below for detail on how to refer patients.
Thank you very much and we look forward to your referrals.
If you are not from Somerset please see alternative pages here.
Table of contents
The NHS Type 2 Diabetes Path to Remission Programme in Somerset
This 12-month service has been commissioned for eligible referred patients in Somerset living with Type 2 diabetes. Delivered by Momenta, it’s based on the DiRECT study which showed this approach could help people lose weight, improve their diabetes control, reduce diabetes-related medication and even achieve remission. Anecdotal feedback also indicates many other patient benefits and, in many cases, reduced use of primary care services.
On average participants lose ~15% of their starting weight.
The 12 month programme has three phases. After an initial introduction session the low calorie diet phase lasts for 12 weeks (patients receive their choice of soups, shakes, bars etc. totalling 8-900 calories per day). They then gradually replace these with ‘real food’ meals over six weeks. Phase 3 comprises ongoing support for the last 8 months to help maintain or build on their weight loss.
Regular in-person group support sessions for 10-15 people at local venues are at the heart of the programme. The 21 sessions start weekly, before moving to fortnightly and then monthly. Led by trained Coaches and based on an expert-developed curriculum, these sessions provide patients with the knowledge, skills and support they need.
If your patients attend the group sessions they will receive all their total diet replacement products (Exante) and a range of high-quality resources including Workbooks, a Lifestyle logbook, online recipe book and 12 months’ premium access to the EXi physical activity app – all free of charge.
Referred patients also require a medications review, with deprescribing in line with NHSE Expert Panel guidelines for many – to be enacted on the day they start the TDR products. 15 minute appointments (in-person or virtual) are recommended for eligibility confirmation, referral discussion including medications adjustment and associated admin.
Referrals can be made on an ad hoc basis, for example at diagnosis or annual reviews. However, as NHS Somerset chose in-person group delivery, multiple referrals per practice are preferable as this minimises patient waiting times and maximises their choice of programme (day, time, location). This webpage includes an EMIS search, auto-populating invitation text/letter and referral forms, as well as guidance on the above and contact details if you have any questions.
We look forward to your referrals and both NHS Somerset and Momenta will be delighted to support in any way we are able.
Identifying interested patients
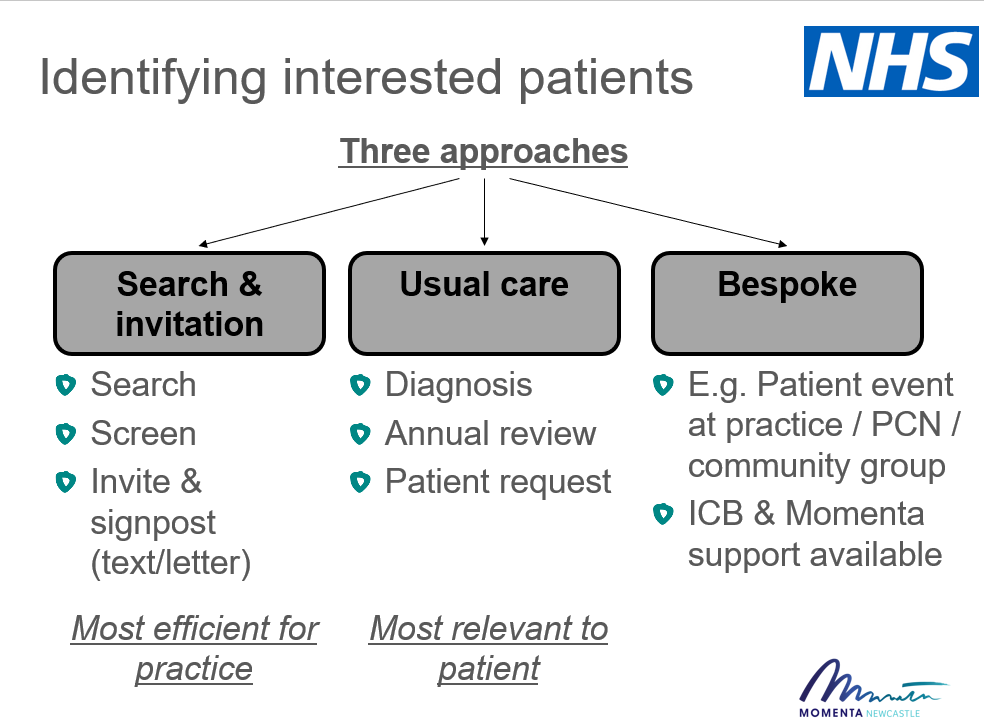
GP practices can choose from three approaches to identifying eligible patients prior to a referral appointment.
In all cases, interested and eligible patients should attend a referral appointment to discuss the programme and any adjustments they should make to their medications on the first day of taking TDR products. The GP practice must then send a completed Referral and Medications Adjustment form to Momenta.
As a guide, 15 minutes should suffice for a patient record review, patient discussion and completing and emailing the referral and medications adjustment form. Although the appointment can be with different healthcare professionals the medications adjustments must be signed off by an appropriate prescriber and clinical responsibility for the patient remains with the GP practice.
See below for supporting information and resources.
Momenta host weekly lunchtime ‘drop-in’ sessions which you can join for an overview of the service or to ask any specific questions.
Participant case studies
Some participants have shared their stories – you might find their experiences help you explain the programme to your patients – or they might just make you smile…
Juliet, Birmingham & Solihull
Eligibility criteria
Inclusion criteria
- Aged between 18-65 inclusive
- Diagnosed with Type 2 diabetes within last 6 years
- BMI of >=27kg/m² (adjusted to >=25kg/m² in people of BAME origin)
- Attended monitoring and diabetes review in last 12 months, incl. retinal screening and commit to continue annual reviews, even if achieve remission. (If newly diagnosed no need to wait for retinal screening before making offer of referral).
- HbA1c within 12 months, with values as follows:
- If on diabetes medication, HbA1c >=43 mmol/mol (6.1%)
- If not on diabetes medication, HbA1c >=48 mmol/mol (6.5%)
- In all cases, HbA1c must be <=87 mmol/mol (10.1%)
Exclusion criteria
- Current insulin user
- Currently breastfeeding
- Pregnant or planning to become pregnant within the next 6 months
- Heart attack or stroke in last 6 months; severe heart failure (New York Heart Association grade 3 or 4); severe renal impairment (most recent eGFR <30mls/min/1.73m2); active liver disease (not including NAFLD); active substance use disorder; active eating disorder (including binge eating); porphyria; or known proliferative retinopathy that has not been treated (not excluding individuals who are newly diagnosed and have not yet had the opportunity for retinal screening).
- Had bariatric surgery
- Health professional assessment that patient is unable to understand or meet the demands and/or monitoring requirements of the NHS Programme; or for whom the programme is not appropriate clinically (consulting with relevant Specialist teams if required); or for whom safe and robust medications adjustment is not practical in a primary care setting.
Patient information
You can send patients to this landing page for more information about the service – this is helpful to do when inviting patients by text (or email).
Alternatively you can download an A4 PDF Patient Information Leaflet for local printing / attachment.
EMIS searches
You can download this EMIS search to obtain a ‘longlist’ of potentially eligible patients with and without mobile phone numbers.
We suggest you screen out patients you believe are ineligible or otherwise inappropriate manually before contacting them directly by text and/or letter and/or phone.
You can also download a one-page summary of how to import the search and which searches to run when you open them i.e.:
- $LCD patient list no mobile (Run this and call/letter)
- $LCD patient list with mobile (Run this and text)
You will need to download the document below then then ‘unzip’ or extract it before using.
We have improved the search to address differences in coding. We extended the timescale for eligible HbA1c readings and diabetes reviews to 18 months (from 12). This will include patients who might have delayed their annual review / blood test but are otherwise eligible. If interested, they can be referred after an updated blood test.
We suggest running the search (as per notes above and instructions). If it returns fewer patients than you expect please contact us as there may be other coding-related avenues to explore.
Finally, we extend our thanks to Scott Greenwood and colleagues at NECS and Joel Wilson at Symphony Healthcare Services for developing the searches and Referral and Medication Adjustment Form as well as colleagues across many practices who have helped refine it.
Patient communications
After a manual screen of the search results GP practices usually send patients further information about the service and ask them to get back in contact if they want to discuss a referral. This step means you only discuss the T2DR programme with patients who are both eligible and interested, saving you and them valuable time.
Some practices send text messages, some letters and others a combination. Some call patients they consider to be priorities.
Steps include:
- Search: Generate ‘longlist of potential referrals.
- Screen: Against non-searchable eligibility and other suitability criteria.
- Contact: By text message, and/or letter and/or call (using your practice’s standard approach and platform e.g. AccuRx, MJog, iPlato etc.
- – Referral and medications adjustment appointments: Diarise with interested patients who request them (possibly in a clinic for efficiency).
The text or letter contact will alert them to the new free NHS Type 2 Diabetes Path to Remission Programme. Texts will link to a landing page https://momentanewcastle.com/patient-lcd-somerset and letters include a leaflet – both with more information about the programme and next steps. Patients are encouraged to contact Momenta with any questions about the programme to reduce burden on your practice.
Sample invitation text and letter, an EMIS template for the letter and a one-page summary on importing documents to EMIS are available below.
Note: You will need to ‘unzip’ or extract the template from the folder it downloads in before importing to EMIS.
Using accuRx to support referrals
Referrers might find it helpful to use the accuRx text messaging system to focus on interested potential referrals. Summary steps include:
– Run Register search to generate ‘longlist of potential referrals
– Conduct manual screen against non-searchable eligibility criteria
– Send potentially eligible patients a bulk text message using accuRx templates
– This will signpost them to https://momentanewcastle.com/introduction where they can find out more about the programme and assess their Readiness before deciding if they would like to talk to you about a referral
– Interested patients can then text back to discuss a referral and associated medications changes
This process should help you discuss the LCD programme only with eligible patents who have expressed interest, saving you and them valuable time.
Referral and Medications Adjustment Form and guides
You can download the EMIS Referral and Medications Adjustment Form here – as well as a one-page summary on importing documents to EMIS.
Please ensure all sections marked essential are completed and that you have discussed any medications adjustments (or lack of them) with each patient before referring.Note: You will need to ‘unzip’ or extract the template from the folder it downloads in before importing to EMIS.
Click here for a ‘how to’ video on making a referral, including the medications adjustment form
Medications adjustments guidelines
Medical Guidance with examples and context from NHS England. This is a comprehensive guide developed by the NHSE&I Expert Advisory Group including clinicians and lead researchers.
We have added an indicative one page overview of NHSE Medical Guidance – and references to relevant sections in the main document – and appended it to the slides.
Click here for a ‘how to’ video on the medications adjustment guidelines
Education session for GP practice referrers - 4/03/2022
Patient readiness (self-)assessment
You can use this standalone patient readiness (self-)assessment to either give to your patient to complete on their own or guide them through it. The patient landing page has a copy embedded. Alternatively you can download this document (for printing / emailing) and also view one-page instructions for healthcare professionals. Please note this has been developed by Momenta’s Clinical Director, a health and clinical psychologist, specifically to support decision-making but it is not an externally validated tool.
Key contacts
Referrals
somicb.lcd@nhs.net
PLEASE DO NOT SEND REFERRALS OR PID TO ANY OTHER EMAIL
Weekly Referrer lunchtime drop-in.
Plain text pls: Momenta host regular lunchtime 'drop-in' sessions which you can join for an overview of the service or to ask any specific questions. Follow this link and click the Contract-specific button.
Jon Scott
Momenta Newcastle
Contract Manager for NHS Type 2 Diabetes Path to Remission Programme, (formerly the NHS Low Calorie Diet Programme)
Email: jon.scott@momentanewcastle.com
Tel: 01823 774 175
Lesley Harper
Somerset ICB
Project Officer Lead for NHS Type 2 Diabetes Path to Remission Programme, (formerly the NHS Low Calorie Diet Programme)
Email: lesley.harper1@nhs.net
SNOMED codes for NHS Type 2 Diabetes Path to Remission Programme
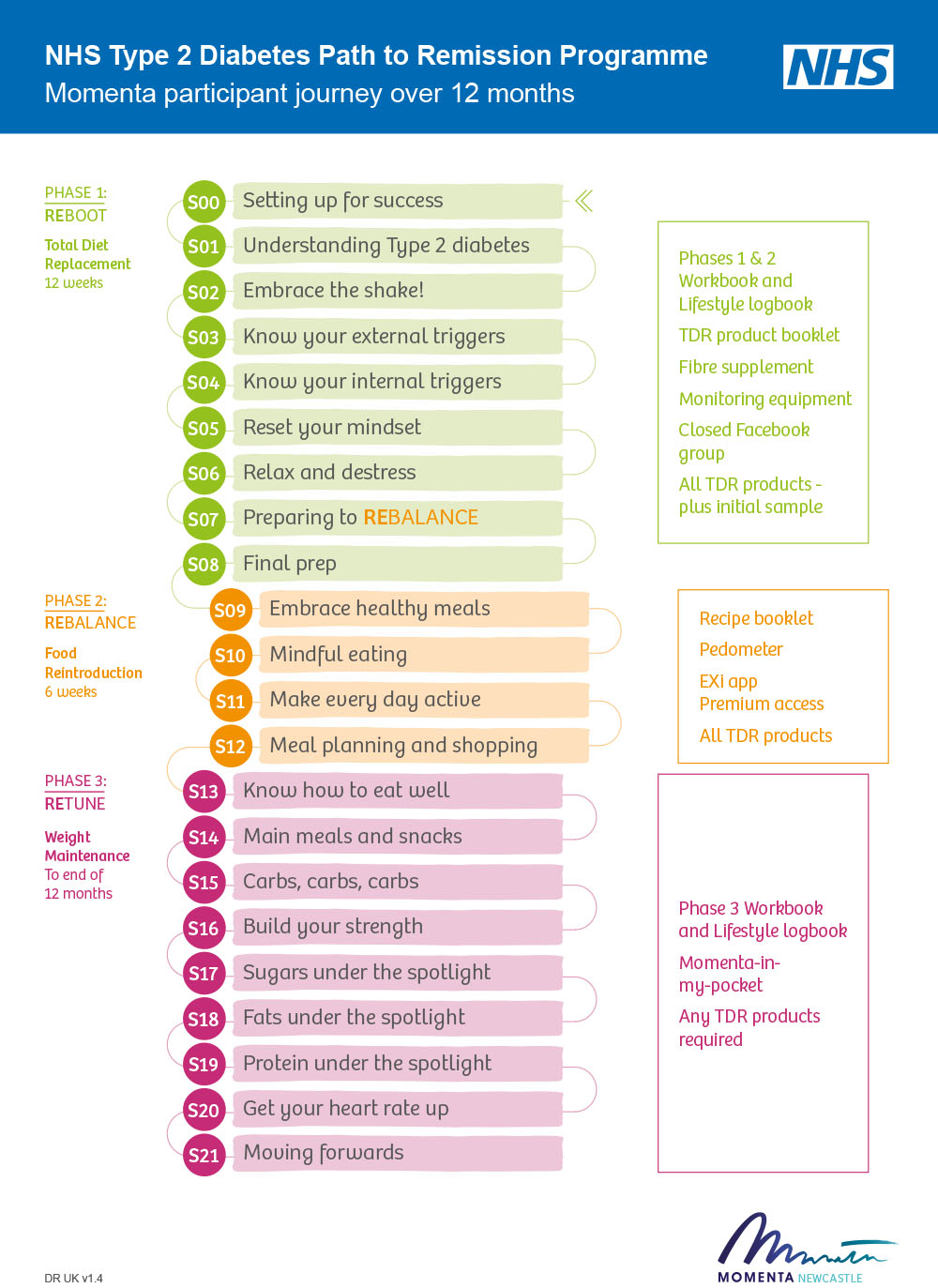
Patient journey
The NHS Type 2 Diabetes Path to Remission Programme is delivered in-person to groups of up to 15 people at community venues. It is a complex three-phase behavioural intervention over 12 months:
- Phase 1 Reboot: Total Diet Replacement (12 weeks)
- Phase 2 Rebalance: Food Reintroduction (6 weeks)
- Phase 3 Retune: Weight Maintenance (until 12 months).
The 75 minute sessions focus on the following topics over the 12 months and include 15 minutes for weight, blood glucose and blood pressure monitoring. Participants also receive a range of resources at different points.
Complaints contacts and procedures
Complaints should be addressed to the Provider (Momenta Newcastle) and/or the CCG and/or the Commissioner (NHS England) as appropriate.
– Momenta Newcastle (Provider): complaints@momentanewcastle.com
https://momentanewcastle.com/complaints
– NHS England: england.diabetestreatment@nhs.net
Referring from a different area?
Momenta also provides the NHS Type 2 Diabetes Path to Remission Programme in other areas, each with their own referral forms, local contacts and minor differences. Please follow the links below for Referrer information from other areas:



